Tummy Tuck for Post-Weight Loss Patients: Managing Excess Skin and Muscle Laxity
Table of Contents
Introduction
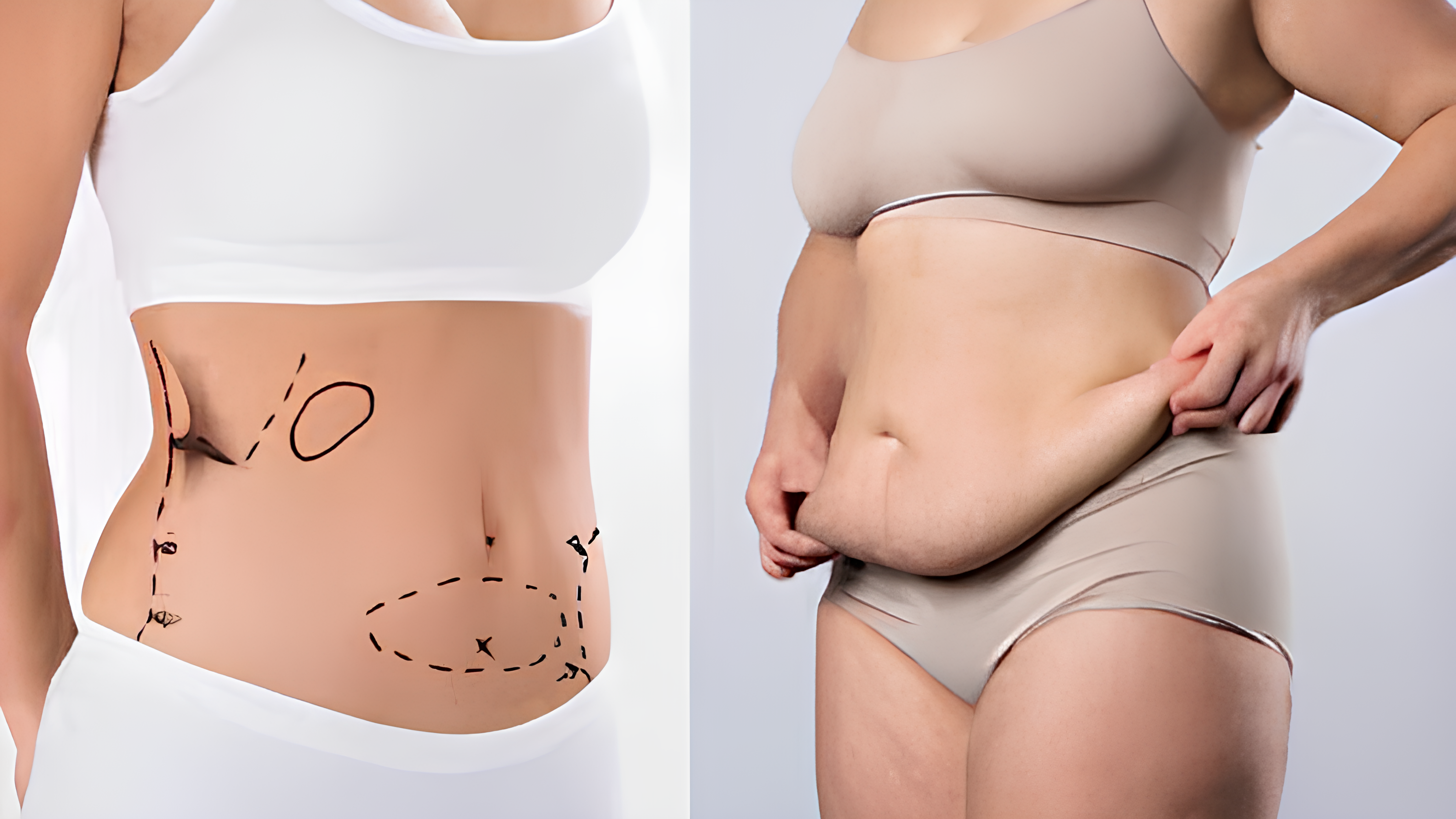
Significant weight loss often results in loose abdominal skin and weakened muscles, creating both functional and aesthetic concerns. Excess skin can cause discomfort and hygiene issues, while weakened abdominal muscles may impair posture and core stability.
Abdominoplasty, commonly known as a tummy tuck, addresses these issues by removing redundant skin and tightening muscles to restore a firmer abdominal profile. This procedure enhances physical comfort, improves appearance, and boosts self-confidence.
This article covers surgical techniques tailored for post-weight loss patients, optimal timing for surgery, and recovery expectations, providing essential information for those considering this transformative procedure.
Addressing Excess Skin Removal in Post-Weight Loss Tummy Tuck Procedures
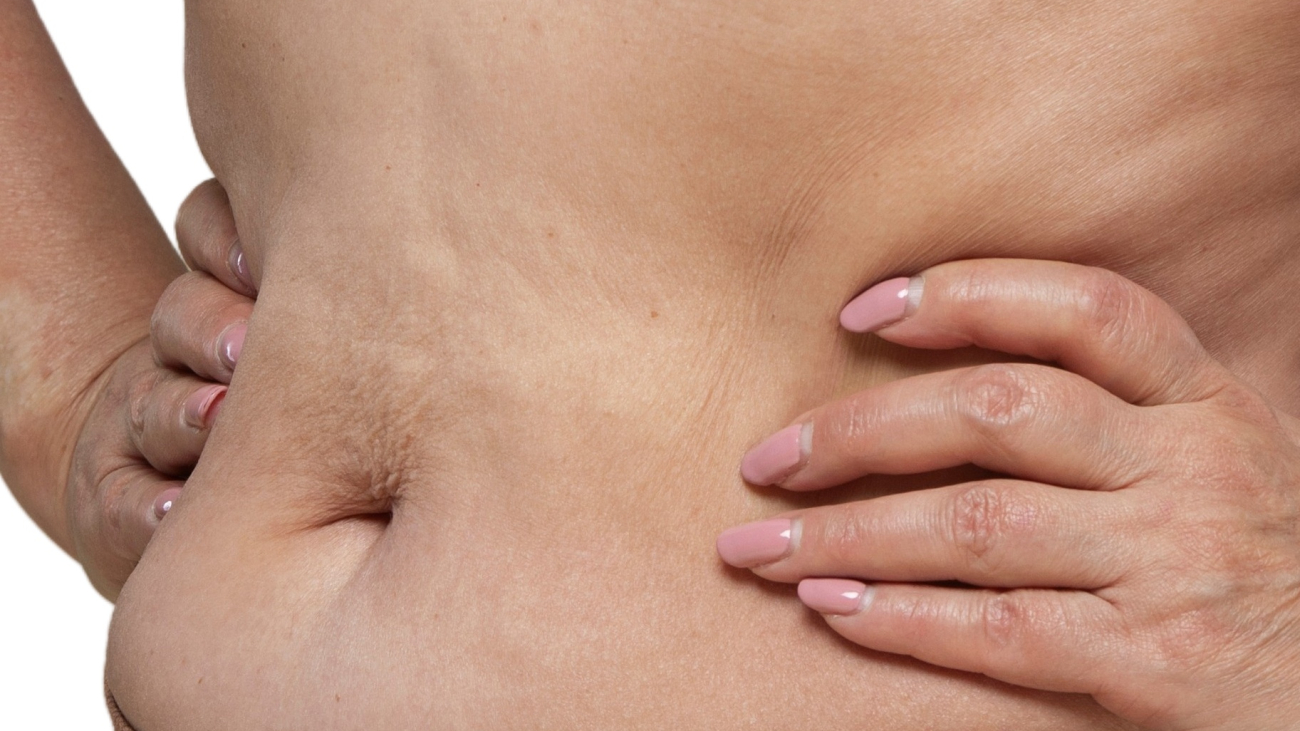
Following major weight loss, the skin often fails to retract due to loss of elasticity and prolonged stretching. A tummy tuck removes this surplus skin, reshaping the abdominal area to achieve a smoother contour.
Important aspects include:
- Excess skin results primarily from skin overstretching during weight gain.
- The amount and location of skin excess guide surgical planning.
- Removal of redundant skin improves mobility and reduces irritation.
- Precise incision placement limits visible scarring.
- The procedure is customized to the patient’s unique anatomy.
By eliminating excess skin, the surgery restores both function and aesthetics, enhancing patient comfort and appearance.
Repairing Muscle Laxity During Abdominoplasty After Major Weight Loss
Abdominal muscle separation, or diastasis recti, frequently accompanies significant weight loss. Repairing this defect is a crucial part of abdominoplasty to restore abdominal wall integrity.
Surgical repair involves:
- Suturing the separated muscles to reinforce core strength.
- Improving posture and reducing associated back discomfort.
- Enhancing the abdominal contour alongside skin removal.
- Adapting techniques based on the extent of muscle laxity.
Addressing muscle laxity optimizes both functional support and cosmetic outcomes after weight loss.
Comparing Extended and Traditional Tummy Tuck Techniques for Skin Laxity
|
Technique
|
Ideal Candidates
|
Skin Laxity Addressed
|
Incision Length
|
|
|---|---|---|---|---|
|
Traditional Tummy Tuck
|
Moderate localized skin excess
|
Targets central abdominal area
|
Standard lower abdominal incision
|
|
|
Extended Tummy Tuck
|
Extensive laxity including flanks
|
Addresses broader skin areas
|
Longer incision extending to sides
|
| Recovery Time | Approximately 2-4 weeks | Depends on surgical extent | Extended procedure requires longer recovery | | Results Longevity | Durable abdominal contour | Comprehensive body shaping | Provides enhanced waistline definition |
Selection depends on the distribution and severity of skin laxity, balancing correction needs with recovery considerations.
Timing Considerations for Tummy Tuck Surgery After Significant Weight Loss
Optimal timing enhances surgical success and healing:
- Surgery is best scheduled after weight has stabilized for several months.
- Avoid operations during ongoing weight loss or fluctuations.
- Allow skin and tissues to adjust naturally before intervention.
- Discuss overall health and lifestyle factors with your surgeon.
- Plan for sufficient recovery and postoperative care.
Appropriate timing minimizes complications and supports lasting results.
Surgical Planning Strategies to Optimize Results in Post-Weight Loss Abdominoplasty
Successful outcomes begin with thorough preoperative evaluation:
- Assess skin quality, fat distribution, and muscle condition.
- Develop an individualized surgical approach tailored to anatomy.
- Employ precise techniques to reduce risks and enhance healing.
- Align surgical goals with patient expectations through detailed consultation.
This comprehensive planning maximizes safety and aesthetic results.
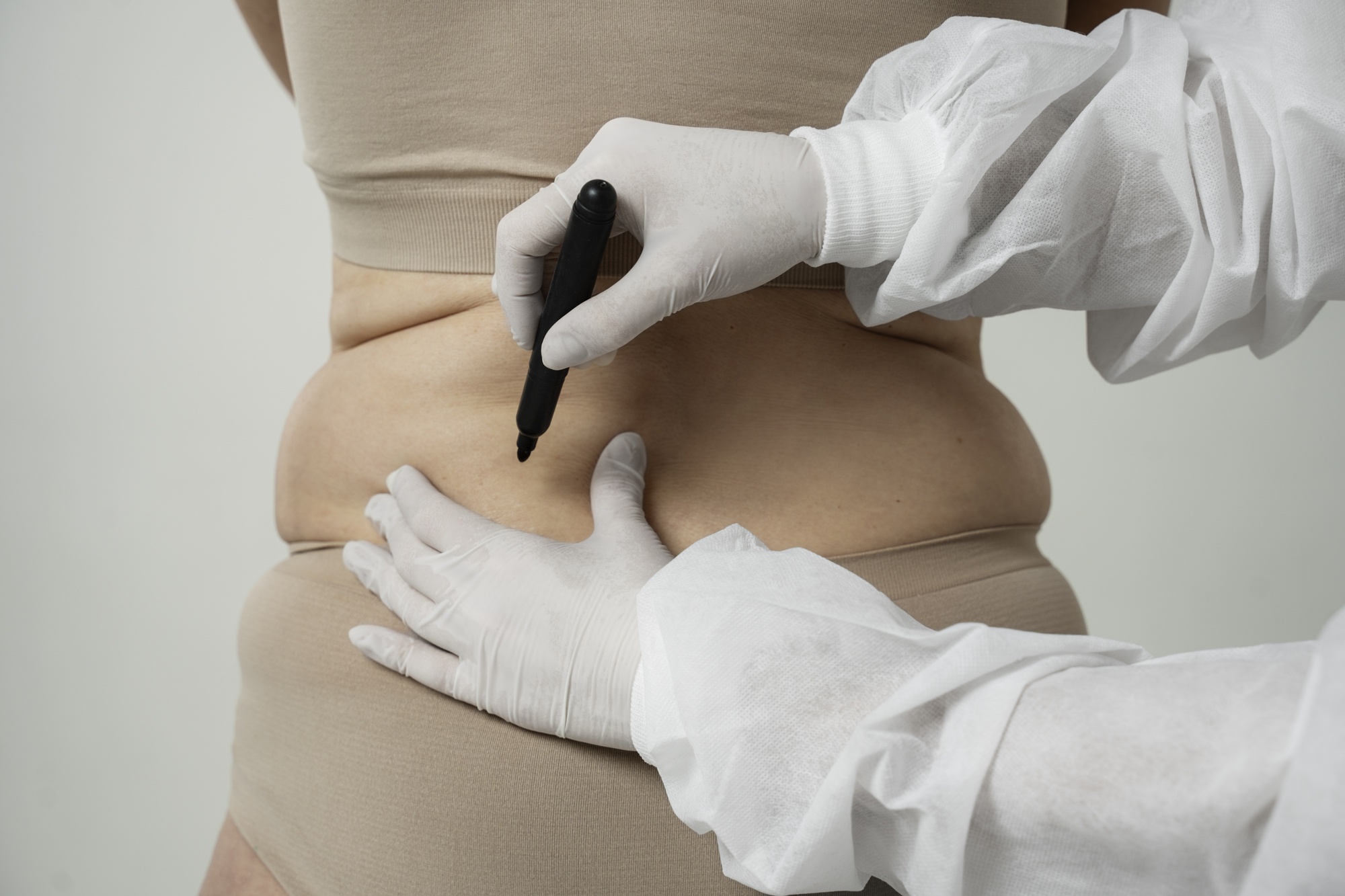
Managing Scar Placement and Healing in Post-Bariatric Tummy Tuck Patients
Scar management techniques focus on minimizing visibility and promoting healing:
- Incisions are placed in natural creases or low on the abdomen.
- Use of layered suturing supports tissue strength and reduces tension.
- Postoperative care includes scar massage and silicone-based treatments.
- Patients receive specific guidance to prevent infection and support recovery.
- Early mobilization improves circulation and wound healing.
These strategies contribute to improved scar outcomes and patient satisfaction.
Impact of Weight Loss Methods on Tummy Tuck Surgical Approach and Outcomes
The nature of prior weight loss influences surgery planning:
- Bariatric surgery patients frequently present with more extensive skin laxity and muscle weakness.
- Weight loss through lifestyle changes may result in less severe skin redundancy but variable muscle tone.
- Surgeons customize techniques considering these differences to optimize healing and aesthetics.
Understanding each patient’s weight loss background helps tailor effective treatment plans.
Balancing Skin Removal Extent With Functional and Aesthetic Goals
Achieving a harmonious balance between skin excision and overall results is essential:
|
Factor
|
Functional Benefit
|
Aesthetic Outcome
|
Consideration
|
|
|---|---|---|---|---|
|
Skin Removal Extent
|
Reduces discomfort, enhances mobility
|
Creates firmer abdominal shape
|
Avoid excessive tension
|
|
|
Muscle Repair
|
Supports core stability
|
Provides flatter abdominal area
|
Customized to muscle condition
|
|
|
Scar Placement
|
Minimizes irritation
|
Conceals scars effectively
|
Strategic positioning
|
|
|
Patient Anatomy
|
Addresses specific laxity patterns
|
Maintains natural proportions
|
Personalized surgical design
|
Tailored planning ensures both comfort and a pleasing appearance.
Postoperative Recovery Challenges Unique to Post-Weight Loss Tummy Tuck Patients
Recovery may involve specific challenges:
- Healing may be slower due to skin quality.
- Risk of infection and scarring requires close monitoring.
- Muscle weakness can limit mobility initially.
- Swelling and fluid retention are common post-surgery.
- Use of compression garments and adjusted pain control aid recovery.
- Gradual resumption of activities supports safe healing.
Awareness of these factors helps prepare patients for the recovery process.
Combining Muscle Repair and Excess Skin Excision for Optimal Contouring
Addressing both muscle laxity and excess skin simultaneously yields superior contouring:
- Muscle repair restores function and core stability.
- Skin excision refines the abdominal silhouette.
- This combined approach respects individual patient anatomy and goals.
- It promotes balanced aesthetic and functional improvements.
Such comprehensive treatment is often essential after significant weight loss.
Evaluating When a Body Lift Is Preferred Over a Tummy Tuck After Weight Loss
Selection between procedures depends on skin excess patterns:
- Tummy tuck focuses on the abdominal region alone.
- Body lifts address circumferential skin redundancy including thighs and buttocks.
- Patient health, prior surgeries, and body shape influence the decision.
- Specialist evaluation ensures the most appropriate surgical plan.
Choosing the correct procedure optimizes overall contouring and recovery.
Long-Term Maintenance and Outcomes Following Muscle and Skin Correction Surgery
Sustaining results involves lifestyle commitment:
- Maintaining a stable weight through balanced diet is crucial.
- Regular physical activity supports muscle tone and abdominal strength.
- Follow-up care allows early identification of any issues.
- Patients benefit from understanding the role of lifestyle in preserving outcomes.
Long-term adherence enhances durability of improvements and patient satisfaction.
Frequently Asked Questions
What surgical techniques are used in a tummy tuck for patients after significant weight loss? Techniques typically include removal of excess skin combined with repair of abdominal muscle separation. The approach is customized based on the extent of skin redundancy and muscle laxity to achieve natural, lasting results.
How does a tummy tuck address excess skin differently after major weight loss? Post-weight loss skin often lacks elasticity and forms folds. The procedure precisely excises this skin and repositions remaining tissue to create a smoother and more comfortable abdominal contour.
Is muscle laxity common after weight loss, and how is it treated during surgery? Muscle separation is frequently seen in these patients. Surgeons repair this by suturing muscles together, restoring core strength and improving posture.
What should patients expect during recovery from a post-weight loss tummy tuck? Recovery includes swelling and discomfort initially, with gradual improvement over weeks. Compression garments and adherence to postoperative instructions facilitate healing and contour refinement.
Can a tummy tuck improve both function and appearance for post-weight loss patients? Yes. The surgery addresses loose skin and muscle laxity, enhancing abdominal strength, mobility, and aesthetic appearance, leading to improved confidence and quality of life.
Clinic Wise is dedicated to providing expert care for patients seeking abdominal contouring after significant weight loss.
Related Posts
Understanding the Relationship Between Tummy Tuck Surgery and Weight Loss
Weight Loss and Tummy Tuck Surgery Examine the impact of stomach tuck surgery on body contouring and weight loss. Discover Read more
Differences between Tummy Tuck and J-Plasma
What is Tummy Tuck? Abdominoplasty, a tummy tuck, is an aesthetic surgical surgery used to enhance the physical appearance and Read more
Discover the Skin Tightening Treatment Option for You
Maintaining smooth, supple skin on your face and body might become more difficult as you age, even with proactive regular Read more