Breast augmentation with nipple reduction represents a comprehensive approach to achieving your ideal breast appearance by addressing both volume and nipple proportion in a single surgical procedure. While breast augmentation increases breast size and enhances shape, combining it with nipple reduction ensures harmonious aesthetics when enlarged or elongated nipples would otherwise detract from your beautiful results. Understanding how these procedures work together, what to expect, and whether this combination suits your unique anatomy empowers you to make informed decisions about achieving balanced, confident, and naturally beautiful breast enhancement.
Many women seeking breast augmentation discover that their nipples are disproportionately large or elongated for their desired breast size. Combining these procedures eliminates the need for staged surgeries, reduces overall recovery time, and ensures your nipples complement your enhanced breast volume perfectly from the moment you heal.
Understanding Breast Augmentation Fundamentals
What Does Augmentation of the Breast Mean?
Breast augmentation, also called augmentation mammoplasty, is a surgical procedure designed to increase breast size, improve shape, and enhance overall breast aesthetics. This transformative surgery addresses various concerns including naturally small breasts, volume loss after pregnancy or weight changes, and breast asymmetry.
Breast Augmentation Achieves:
- Increased breast volume and projection
- Enhanced breast shape and contour
- Improved breast symmetry
- Better proportion with body frame
- Restored volume after life changes
- Increased confidence and self-image
What Is the Difference Between Breast Implants and Breast Augmentation?
This common question deserves clear explanation:
Breast Implants: Medical devices (silicone gel or saline-filled) used to increase breast size. They are the tools or materials used in the procedure.
Breast Augmentation: The complete surgical procedure that increases breast size, which may utilize implants, fat transfer, or combination approaches. It’s the overall process and technique.
The Relationship: Breast implants are one method used to achieve breast augmentation. Think of it this way: breast augmentation is the goal and procedure, while breast implants are one of the means to accomplish that goal.
Alternative Augmentation Methods:
- Breast augmentation with fat transfer: Using your own fat harvested via liposuction
- Composite augmentation: Combining implants with fat grafting
- Hybrid techniques: Utilizing multiple approaches for optimal results
Why Combine Nipple Reduction with Breast Augmentation?
The Aesthetic Advantage
Proportional Harmony:
Breast augmentation increases breast volume, but this enhancement can make disproportionately large nipples appear even more prominent. Combining procedures ensures:
Balanced Proportions Nipple size remains harmonious with enlarged breast volume.
Enhanced Aesthetics Both breast shape and nipple appearance contribute to beautiful, natural-looking results.
Immediate Complete Results Achieve your ideal breast appearance without requiring future revision surgery.
Optimal Symmetry Address both breast and nipple asymmetries simultaneously for comprehensive correction.
Practical Benefits
Single Recovery Period: One surgery means one healing process instead of two separate recovery experiences.
Cost Efficiency: Combined procedures are typically more economical than staging surgeries separately.
Reduced Anesthesia Exposure: Undergo anesthesia once rather than multiple times for separate procedures.
Faster Total Timeline: Achieve complete transformation sooner without waiting between staged surgeries.
Common Nipple Concerns Addressed
Enlarged Nipples: Nipples with excessive diameter that appear disproportionate to breast size.
Elongated Nipples: Nipples with excessive projection extending outward prominently.
Combined Issues: Both diameter and projection concerns requiring comprehensive reshaping.
Asymmetrical Nipples: Differences between left and right nipple size, shape, or projection.
The Combined Procedure: What to Expect
Surgical Planning and Customization
Comprehensive Assessment:
During your consultation at Clinic Wise, our board-certified plastic surgeons evaluate:
Breast Characteristics:
- Current breast size and shape
- Chest wall dimensions
- Tissue quality and skin elasticity
- Existing asymmetries
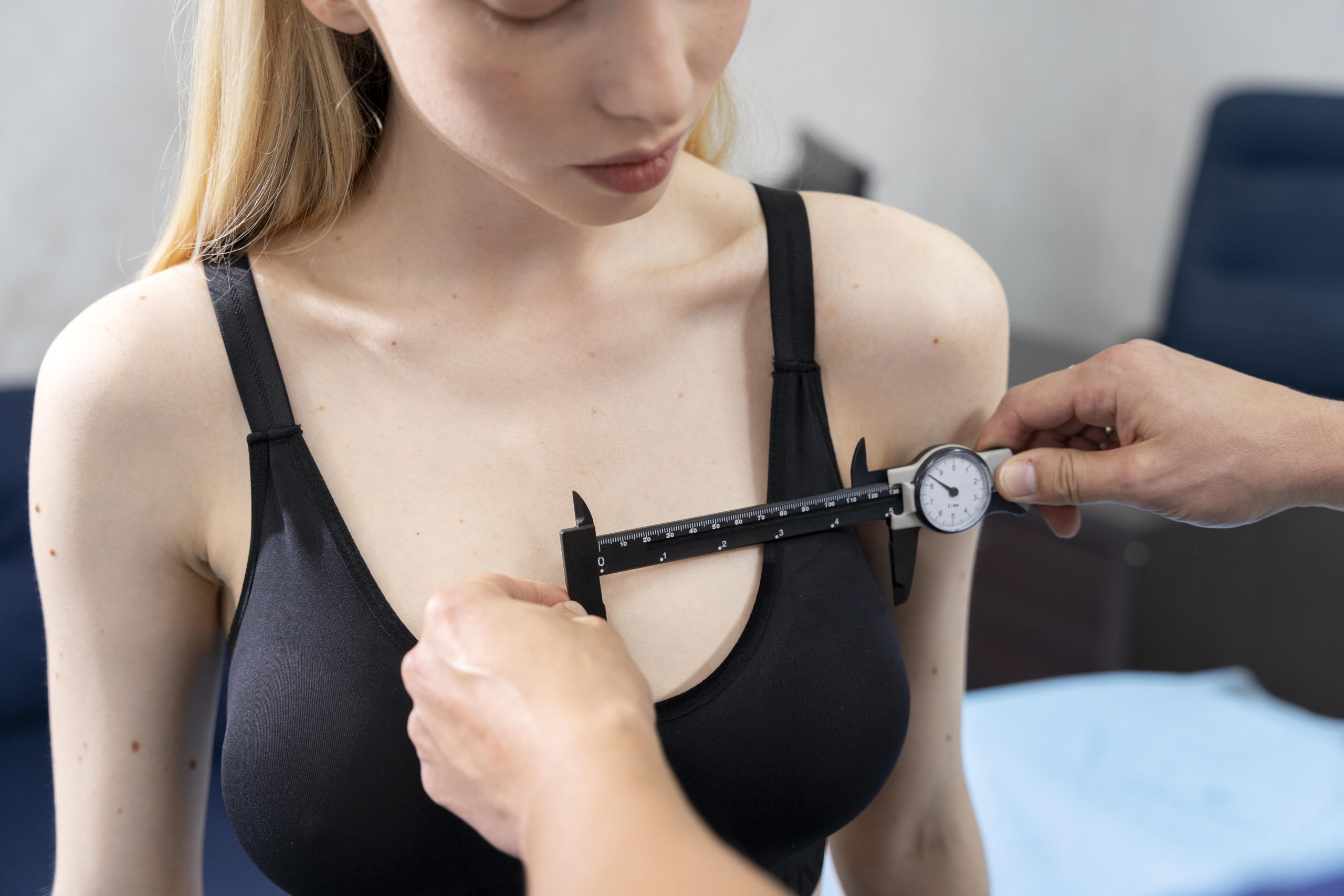
Nipple Evaluation:
- Diameter measurement
- Projection assessment
- Areola size and shape
- Symmetry between sides
Goal Discussion:
- Desired breast size increase
- Ideal nipple proportions
- Natural vs. enhanced appearance preferences
- Lifestyle and activity considerations
Breast Augmentation Component
Implant Selection Process:
Size Determination: Using breast augmentation sizers during consultation helps visualize potential outcomes and select optimal implant volume for your frame and goals.
Implant Type Selection:
- Silicone gel implants (most popular for natural feel)
- Saline implants (adjustable, slightly firmer)
- Gummy bear implants (form-stable, shaped)
- Round vs. anatomical shapes
Placement Options:
- Submuscular (under pectoral muscle)
- Subglandular (under breast tissue)
- Dual plane (combination approach)
Incision Location:
- Inframammary (breast fold) – most common
- Periareolar (around nipple) – convenient for nipple reduction
- Transaxillary (armpit)
- Transumbilical (belly button) – rarely used
Nipple Reduction Component
Surgical Technique:
Diameter Reduction: Removing a circular band of tissue around the nipple’s perimeter to decrease overall size.
Projection Reduction: Removing tissue from the nipple tip to reduce forward extension.
Reshaping: Sculpting remaining tissue for aesthetically pleasing, natural-appearing nipple contour.
Combined Approach: Addressing both diameter and projection when necessary for optimal proportions.
The Surgical Process
Procedure Timeline:
Combined Surgery Duration: 2-3.5 hours typically
Anesthesia: General anesthesia for patient comfort and optimal surgical conditions.
Surgical Steps:
- Breast augmentation performed first
- Implants placed and positioned
- Nipple reduction completed while tissues are accessible
- Meticulous closure with dissolvable sutures
- Surgical dressings and supportive bra application
Hospital Stay: Most patients go home the same day, though overnight observation is sometimes recommended.
Breast Augmentation with Lift
Many patients considering breast augmentation discover they also need a lift:
Understanding Breast Lift Necessity
When Lift Is Recommended:
Significant Sagging (Ptosis): Nipples positioned below the breast fold indicate the need for lifting.
Downward-Pointing Nipples: Nipples pointing toward the floor rather than forward suggest sagging requiring correction.
Loss of Upper Pole Fullness: Deflated appearance in the upper breast area benefits from both implants and lifting.
Asymmetrical Positioning: Different breast heights or nipple positions require lift for symmetry.
Lift Techniques Combined with Augmentation
Crescent Lift: Minimal lifting through small incision along upper areola border.
Periareolar (Donut) Lift: Moderate lifting with circular incision around the areola.
Vertical (Lollipop) Lift: More substantial lifting with vertical scar from areola to breast fold.
Anchor (Inverted-T) Lift: Maximum lifting for severe sagging with anchor-shaped scar pattern.
Triple Combination: Augmentation + Lift + Nipple Reduction
Some patients benefit from all three procedures simultaneously:
Comprehensive Transformation:
- Increased volume from implants
- Elevated position from lift
- Proportional nipples from reduction
Complex but Rewarding: While technically demanding, this combination delivers complete breast rejuvenation in a single surgery when performed by experienced, board-certified plastic surgeons.
Breast Augmentation with Fat Transfer
An alternative or complementary approach to implant-based augmentation:
Understanding Fat Transfer Augmentation
The Process:
Fat Harvesting: Liposuction removes fat from areas with excess (abdomen, thighs, flanks).
Fat Processing: Harvested fat is purified and prepared for injection.
Strategic Injection: Processed fat is carefully injected throughout breast tissue in multiple layers.
Natural Integration: Successfully transferred fat becomes permanent living tissue.
Fat Transfer Advantages
100% Natural Material: Your own tissue eliminates foreign body concerns.
Dual Body Contouring: Removes unwanted fat while enhancing breasts simultaneously.
Natural Look and Feel: Results feel completely natural to touch.
No Implant-Related Issues: Avoids capsular contracture, rupture, or rippling concerns.
Fat Transfer Limitations
Modest Size Increase: Typically achieves one cup size increase per procedure.
Multiple Sessions Possible: Larger increases may require staged treatments.
Fat Reabsorption: 30-50% of transferred fat may not survive permanently.
Donor Site Requirements: Adequate body fat necessary for meaningful augmentation.
Combining All Three: Implants + Fat Transfer + Nipple Reduction
Hybrid Augmentation Approach:
Optimal Results:
- Implants provide base volume and projection
- Fat grafting adds natural upper pole fullness
- Nipple reduction ensures proportional aesthetics
Enhanced Natural Appearance: Fat grafting softens implant edges and transitions for seamless, natural-looking results.
Comprehensive Transformation: Addresses volume, shape, contour, and nipple proportion simultaneously.
Breast Augmentation Sizers
A crucial tool in your surgical planning process:
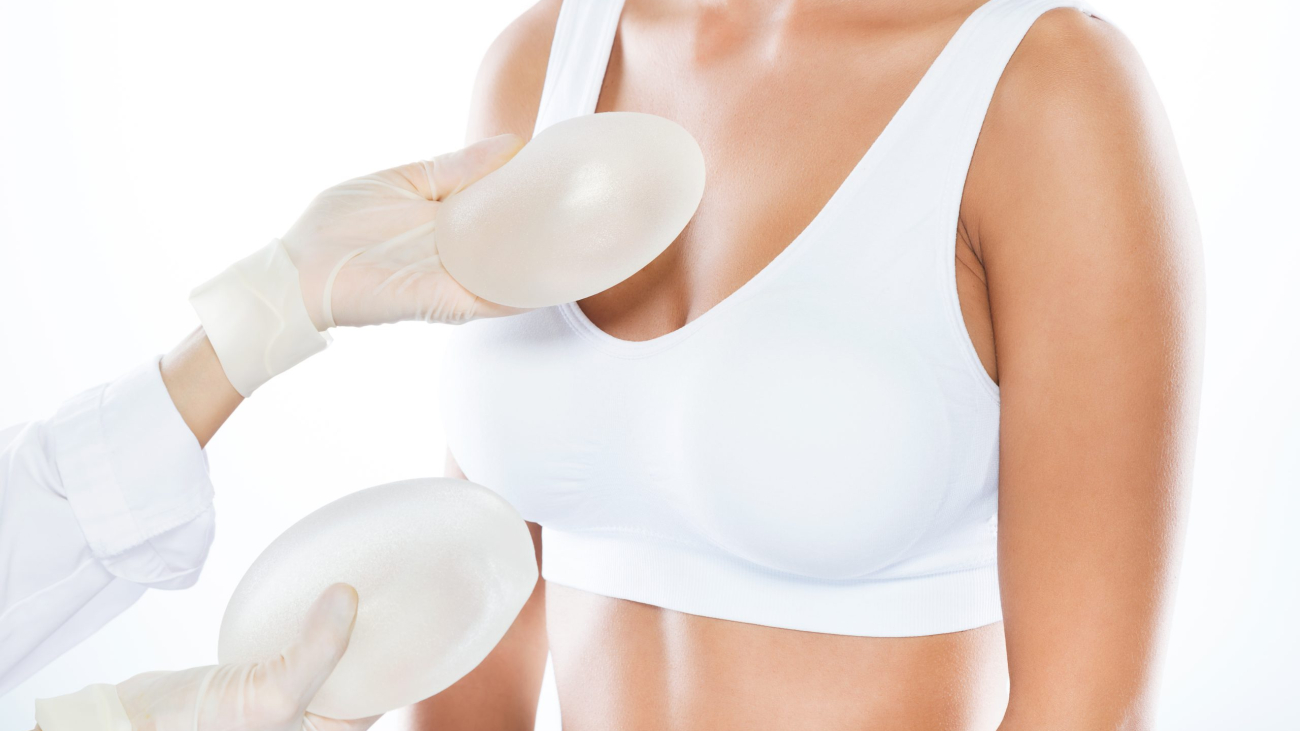
What Are Breast Augmentation Sizers?
Breast augmentation sizers are specialized sizing implants placed inside surgical bras during consultation, allowing you to preview potential results before committing to specific implant sizes.
Sizer Benefits:
Visual Preview: See how different volumes look on your frame in real-time.
Clothing Assessment: Try on your own tops and bras to evaluate fit with various sizes.
Proportion Evaluation: Determine which size creates the balance you desire with your body.
Confidence Building: Reduce decision anxiety by experiencing sizes before surgery.
Partner Input: Involve significant others in the decision-making process if desired.
Using Sizers During Consultation
The Sizer Session Process:
Initial Recommendations: Based on measurements and goals, your surgeon suggests starting size ranges.
Progressive Sizing: Try multiple volumes, typically ranging from conservative to more dramatic.
Movement Assessment: Walk, sit, and move naturally to evaluate how different sizes feel.
Mirror Evaluation: View yourself from all angles in full-length mirrors.
Photography: Many clinics allow photos for home review and decision-making.
Making Your Final Decision
Factors to Consider:
Lifestyle Compatibility: Choose sizes compatible with your activity level and daily life.
Natural vs. Enhanced: Decide where you fall on the natural-to-enhanced appearance spectrum.
Body Frame Proportion: Ensure selected size harmonizes with your overall physique.
Clothing Goals: Consider how you want clothing to fit and what styles you prefer.
Long-Term Satisfaction: Think beyond immediate desires to long-term comfort and happiness.
Professional Guidance: Trust your surgeon’s expertise when recommendations differ from initial preferences.
What Types of Breast Implants Are Most Popular for Natural Results?
Achieving natural-looking augmentation depends on proper implant selection:
Most Natural Implant Characteristics
Silicone Gel Implants – The Gold Standard:
Why Silicone Appears Most Natural:
Cohesive Gel Feel: Modern silicone gel mimics natural breast tissue consistency more closely than saline.
Natural Movement: Silicone implants move and shift like natural breasts during activity.
Reduced Rippling: Less visible rippling or wrinkling compared to saline, especially in thin patients.
Soft Texture: The gel provides softness resembling natural breast tissue.
Size Selection for Natural Results
Moderate Profile Implants:
Natural Projection: Moderate profile implants provide balanced forward projection without excessive roundness.
Proportional Width: Width matches natural breast base dimensions for seamless integration.
Subtle Enhancement: Creates noticeable but not dramatic change in breast size.
Placement for Natural Appearance
Submuscular Placement:
Enhanced Natural Look: Muscle coverage provides smoother upper pole transition and more natural slope.
Better Concealment: Implant edges less visible, especially in thin patients.
Reduced Rippling: Additional tissue layer minimizes visible rippling.
Shape Considerations
Round vs. Anatomical:
Round Implants:
- Provide upper pole fullness
- Natural appearance when properly sized
- Less concern about rotation
- Most popular for augmentation
Anatomical (Teardrop) Implants:
- Shaped to mimic natural breast contour
- Less upper pole fullness
- May appear more natural in some cases
- Risk of rotation affecting appearance
Customization at Clinic Wise
Our board-certified plastic surgeons consider your unique anatomy, tissue characteristics, and aesthetic goals to recommend implant specifications that deliver the natural-looking results you desire. We never use a one-size-fits-all approach.
Book your free online consultation to discuss which implant types and characteristics will create the most natural, beautiful results for your body.
What Is the Best Age for Breast Augmentation?
Timing your breast augmentation appropriately ensures optimal results and satisfaction:
Medical and Legal Considerations
Minimum Age Requirements:
FDA Guidelines:
- Saline implants: Age 18 minimum
- Silicone gel implants: Age 22 minimum
- Fat transfer augmentation: Age 18 minimum
Physical Maturity: Breasts should be fully developed before augmentation surgery.
Ideal Age Ranges
Ages 22-35: Most Common
Why This Range Is Popular:
Physical Development Complete: Breast growth finished, providing stable foundation for augmentation.
Life Stage Appropriate: Often before or between pregnancies, allowing optimal timing.
Good Tissue Quality: Younger skin typically has excellent elasticity for beautiful results.
Long-Term Enjoyment: Decades ahead to appreciate investment and results.
Financial Readiness: Established careers enable investment in aesthetic goals.
Younger Patients (Ages 18-22)
Considerations:
Emotional Maturity: Ensure decision-making capacity and realistic expectations.
Body Changes: Weight fluctuations common at this age may affect results.
Implant Limitations: Restricted to saline implants until age 22 by FDA.
Future Changes: Pregnancy and life changes ahead may impact longevity.
Mature Patients (Ages 35-50+)
Advantages:
Life Stability: Completed childbearing, established lifestyle, stable weight.
Clear Goals: Well-defined aesthetic objectives and realistic expectations.
Appreciation: Often deeply satisfied having achieved long-desired enhancement.
Combination Procedures: May benefit from augmentation with lift due to natural aging changes.
Pregnancy Considerations
Before Pregnancy: Augmentation before pregnancy is safe, though subsequent pregnancies may affect results.
After Pregnancy: Waiting 6-12 months after breastfeeding completion allows breast tissue stabilization.
Between Pregnancies: Personal choice, though additional pregnancies will impact results.
Individual Assessment Priority
Rather than focusing on chronological age, ideal candidates have:
- Fully developed breasts
- Realistic expectations
- Good overall health
- Stable weight for 6+ months
- Completed major life planning (if desired)
- Financial readiness
- Emotional maturity
Schedule your free online consultation with Clinic Wise to determine if now is the right time based on your unique circumstances and goals.
Recovery and Results Timeline
Immediate Post-Operative Period (Days 1-7)
What to Expect:
Discomfort Level: Moderate soreness and tightness, well-managed with prescribed medication.
Swelling and Bruising: Universal and expected, peaking around days 2-3 then gradually improving.
Restricted Movement: Limited arm elevation and activity to protect healing tissues.
Surgical Bra: Continuous wear of supportive surgical bra without underwire.
Nipple Healing: Sensitivity changes, temporary numbness, and initial scar formation.
Early Recovery (Weeks 2-4)
Progressive Improvement:
Reduced Discomfort: Transition to over-the-counter pain management for most patients.
Decreased Swelling: Breast shape becomes more apparent as swelling resolves.
Increased Mobility: Gradual return to light daily activities and gentle arm movement.
Return to Work: Most patients resume desk jobs within 1-2 weeks.
Nipple Sensation: Gradual return of normal sensation, though changes may persist for months.
Intermediate Healing (Months 2-3)
Visible Transformation:
Implant Settling: Breasts drop into natural position as tissues relax and adapt.
Shape Refinement: Final breast contour becomes apparent as swelling completely resolves.
Scar Maturation: Nipple reduction scars fade from red/pink to pale, thin lines.
Exercise Resumption: Cleared for full activity including upper body and chest workouts.
Final Results (Months 6-12)
Complete Healing:
Optimal Appearance: Final breast size, shape, and nipple proportions fully established.
Natural Feel: Breasts feel soft and natural, especially with silicone implants.
Mature Scars: Nipple reduction scars faded to barely visible, thin lines around areola border.
Full Sensation: Most sensation changes resolved, though some areas may remain altered.
Risks and Considerations
General Breast Augmentation Risks
Temporary Issues:
- Swelling, bruising, discomfort (universal, resolves)
- Temporary numbness or sensitivity changes
- Asymmetry during healing phase
Uncommon Complications:
- Infection requiring antibiotics
- Hematoma or seroma (fluid collection)
- Capsular contracture (scar tissue tightening)
- Implant malposition requiring revision
Long-Term Considerations:
- Implant replacement likely within 10-20 years
- Potential revision surgery needs
- Imaging challenges for breast cancer screening
Nipple Reduction Specific Risks
Sensation Changes: Temporary or rarely permanent altered nipple sensation.
Breastfeeding Impact: Potential reduction in milk duct function affecting future breastfeeding.
Scarring: Visible scars around areola border, though typically fade well.
Size Changes: Nipples may appear larger or smaller during healing before final size stabilizes.
Minimizing Risks at Clinic Wise
Our board-certified plastic surgeons’ extensive experience, combined with JCI-accredited facilities and comprehensive protocols, dramatically reduces complication risks while maximizing beautiful, natural results.
Why Choose Clinic Wise for Your Breast Augmentation
Board-Certified Expertise
All breast augmentation procedures performed by plastic surgeons with:
- International board certification
- Extensive breast surgery specialization
- Thousands of successful augmentation procedures
- Advanced training in complex combinations
Comprehensive Approach
We address all aspects of breast aesthetics:
- Volume enhancement through implants or fat transfer
- Proportional nipple and areola sizing
- Lift integration when beneficial
- Customized technique selection
Natural Result Focus
Our surgical philosophy prioritizes:
- Proportional, harmonious outcomes
- Natural movement and feel
- Seamless integration with body
- Appropriate size for frame
Advanced Technology
Access to cutting-edge tools and techniques:
- Latest generation implant options
- Breast augmentation sizers for decision confidence
- State-of-the-art surgical equipment
- Advanced pain management protocols
Exceptional Value
World-class breast augmentation with nipple reduction at approximately one-third of UK prices:
- No quality or safety compromise
- Board-certified surgeon expertise
- JCI-accredited surgical facilities
- All-inclusive transparent pricing
Medical Tourism Excellence
Specialized international patient experience:
- English-speaking coordinators and staff
- Comprehensive travel and logistics management
- Comfortable accommodation arrangements
- Seamless journey from consultation to recovery
Proven Beautiful Results
Extensive before and after portfolio demonstrating:
- Consistent natural-looking outcomes
- Proportional nipple sizing
- High patient satisfaction
- Diverse body types and goals
Preparing for Your Consultation
Before Your Appointment
Gather Information:
- Current bra size and fit concerns
- Photos of breast appearances you admire
- Questions about procedures and techniques
- Medical history and medication list
Document Your Goals:
- Desired size increase
- Natural vs. enhanced preference
- Nipple proportion concerns
- Lifestyle and activity considerations
Research and Educate:
- Review breast augmentation basics
- Understand realistic outcome expectations
- Learn about implant types and options
- Consider your long-term goals
During Your Consultation
Comprehensive Evaluation:
Our surgeons assess:
- Current breast size, shape, and symmetry
- Nipple and areola proportions
- Skin quality and tissue characteristics
- Chest wall dimensions
- Overall body proportions
Treatment Planning:
Receive personalized recommendations for:
- Optimal implant size, type, and placement
- Nipple reduction necessity and approach
- Lift consideration if beneficial
- Fat transfer complementary enhancement
Sizer Experience:
Use breast augmentation sizers to:
- Visualize potential outcomes
- Compare different volumes
- Assess proportion with your frame
- Build decision confidence
Financial Clarity:
Understand complete investment including:
- Transparent pricing breakdown
- All-inclusive package details
- Exceptional value compared to UK costs
- Payment options and financing
Conclusion: Your Path to Beautiful, Proportional Breasts
Breast augmentation with nipple reduction offers a comprehensive solution for achieving perfectly proportioned, naturally beautiful breast enhancement in a single surgical procedure. By addressing both volume and nipple aesthetics simultaneously, you eliminate the need for staged surgeries while ensuring harmonious results from the moment you heal.
Whether you’re considering traditional implant augmentation, breast augmentation with fat transfer, or breast augmentation with lift, our board-certified plastic surgeons at Clinic Wise customize every aspect of your procedure to match your unique anatomy and aesthetic goals. The addition of nipple reduction ensures your enhanced breasts have proportional, attractive nipple dimensions that complement rather than detract from your beautiful new contours.
Understanding what augmentation of the breast means, the difference between breast implants and breast augmentation, and what types of breast implants create the most natural results empowers you to make confident decisions. Combined with expert guidance on the best age for breast augmentation and comprehensive use of breast augmentation sizers during planning, you can move forward with complete clarity and realistic expectations.
At Clinic Wise, our commitment to surgical excellence, natural-looking results, and patient satisfaction—all at approximately one-third of UK prices—makes transformative breast enhancement both accessible and affordable without compromising quality or safety.
Book Your Free Online Consultation with Clinic Wise Today
Take the first step toward the beautiful, proportional breasts you’ve always desired. During your no-obligation virtual consultation, you’ll receive:
- Comprehensive assessment of your breast and nipple concerns
- Personalized recommendations for augmentation approach
- Expert guidance on implant selection for natural results
- Virtual breast augmentation sizer experience
- Honest evaluation of whether nipple reduction enhances your outcome
- Transparent pricing at approximately one-third UK costs
- Extensive before and after examples from similar patients
- Clear understanding of procedure, recovery, and realistic results
Don’t wait to achieve the confident, beautiful breast appearance you deserve. Contact Clinic Wise now to schedule your free online consultation and discover how exceptional, natural-looking breast augmentation results can be with our board-certified surgical expertise and unmatched value.
Your transformation journey begins with a conversation. Book your free consultation today and let us show you how accessible beautiful, proportional results can be.